
Wilmington (937) 382-2347
Fax
(513) 932-1606

Wilmington (937) 382-2347
Fax
(513) 932-1606
Tendons are fibrous tissues that connect muscles with bone. The Achilles tendon is the largest tendon in the body. It connects the calf muscles at the back of the leg with the heel, and facilitates movements such as jumping, running, and walking.
Because the Achilles tendon is engaged so frequently and bears a great deal of pressure and stress throughout the day, it can become injured. Achilles tendon injuries cause the tissue to become irritated, inflamed, and swollen. Pain can come on gradually or be immediate, and will vary from mild to severe depending upon the injury. Where the pain occurs will vary as well, from just above the heel up through the back of the leg. There may also be stiffness in the tendon.
Achilles tendon injuries can often be caused by repetitive stress. They may also occur while running, playing tennis, gymnastics, football, basketball, dancing, soccer, baseball or other sports that require speeding up, slowing down, or pivoting quickly. Wearing high heels, falling from an elevation, stepping in a hole, having flat feet, bone spurs, tight leg muscles or tendons, wearing improper athletic shoes, exercising on uneven surfaces, or starting a new type of exercise can also cause Achilles tendon injuries.
The two most common Achilles tendon injuries are tendonitis and ruptures. Tendonitis causes painful inflammation and can occur in different parts of the tendon. Non-insertional Achilles tendonitis occurs when the fibers in middle of the tendon begin to break down, thicken, and swell. This condition typically affects younger, more active adults. Insertional Achilles tendonitis occurs where the tendon inserts into the heel bone. It is common for bone spurs to form with this type of injury. This condition can affect people of any age and level of activity.
Achilles tendon ruptures are a tear in the tendon. These breaks may be partial or complete. There may be an audible popping noise at the moment of injury and the pain will be sudden and severe.
An Achilles tendon injury can be diagnosed by your podiatrist after they examine you, check your range of motion, and possibly perform a calf squeeze test or review an X-ray or MRI. Depending on the type and severity of your injury, your podiatrist may treat your condition with rest/ice/compression/elevation (RICE), nonsteroidal anti-inflammatory medications, heel lifts, and stretching and strengthening exercises. If you have torn your Achilles tendon, treatment may include physical therapy, ultrasound, shockwave therapy, or possibly even surgery.
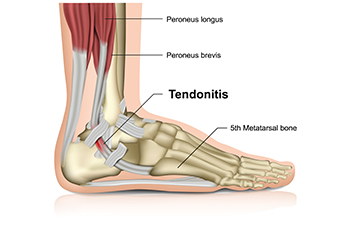
Anyone who has experienced an Achilles tendon injury is all too familiar with the intense pain this condition can cause. This is considered to be the largest tendon in the body, and its function is to connect the calf muscles to the heel. It is responsible for pushing off while walking, running, and jumping, in addition to pointing and flexing the foot. Many patients have heel pain with this type of injury, and it can happen from overuse. People who increase speed and mileage too quickly while running may be prone to a partial or fully ruptured Achilles tendon. Additionally, it may happen from standing on uneven surfaces for most of the day, or possibly from wearing shoes that do not fit correctly. This may help to weaken the tendon, and may gradually lead to the development of this type of injury. The symptoms can include tenderness in the calf and heel area, and it is often difficult to walk. It typically takes several months for this type of injury to completely heal and lifestyle changes may need to occur to avoid stress on the Achilles tendon. If you suffer from an Achilles tendon injury, it is strongly advised that you seek the counsel of a podiatrist who can offer you the correct treatment practices.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Dr. Gerald Perelman of Ohio. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
Rupture Symptoms
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
If you have any questions please feel free to contact our office located in Wilmington, OH . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
A plantar fibroma is a knot in the arch of the foot. It can cause pain when repeated pressure is applied by walking barefoot or wearing tight shoes. While plantar fibromas can appear in anyone, men who are middle-aged or older are said to be more susceptible. The main symptom of a plantar fibroma is a firm lump on the arch of the foot. If there is pain, it can be intensified by putting pressure on the nodule. The lump can stay one size or grow larger. You may have one or more fibromas in the feet and there tends to be a high incidence of recurring plantar fibromas. Generally, a plantar fibroma can be treated without surgery. Treatment might include steroid injections to help shrink the lump, orthotics to help redistribute weight away from the nodule, plantar fascia stretching, or physical therapy to help use anti-inflammatory medication on the lump. If a lump grows larger or more painful, a podiatrist can be consulted to confirm the diagnosis. The doctor will palpate the lump and this may cause pain that can be felt all the way to the toes. An X-ray, MRI, or biopsy might be done if further evaluation is necessary. A lump in the arch of the foot might be something other than a plantar fibroma, such as cysts, nerve or fatty tumors, swollen tendons, or an infection in the foot. It is important to see a podiatrist for proper diagnosis and treatment of plantar fibromas.

The plantar fascia is located on the sole of the foot and it connects the toes to the heels. Some patients may experience a growth that develops inside the plantar fascia, which is often benign. This is referred to as a plantar fibroma that might cause pain while walking and running. It is noticeable by the lump that forms on the bottom of the foot, generally in the center of the arch. The majority of experts agree it occurs due to genetic reasons or medical conditions like epilepsy, diabetes, and alcoholism. Other people can argue a plantar fibroma may develop after an injury occurs to the plantar fascia and the lump may be a natural reaction to the stress from the trauma. Mild relief may be found when the shoes that are worn have extra cushioning, or it may be beneficial to wear custom-made orthotics. If you have developed this condition it is advised that you are under the care of a podiatrist who can provide the treatment options that are correct for you.
A plantar fibroma may disrupt your daily activities. If you have any concerns, contact Dr. Gerald Perelman of Ohio. Our doctor can provide the care you need to keep you pain-free and on your feet.
Plantar Fibroma
A plantar fibroma is a fibrous knot in the arch of the foot. It is embedded in the plantar fascia which is a band of tissue that extends from the heel to the toes along the bottom of the foot. There can be multiple plantar fibromas in the feet at the same time. There are no known causes for this condition. If you have a plantar fibroma, there will be a bump in the arch of your foot that cannot be missed. Any associated pain is most often due to a shoe rubbing against the nodule. Non-surgical options, such as steroid injections, physical therapy, and orthotics should be tried first. Surgery is a last resort and is the only thing that will remove a plantar fibroma entirely. Consult with a podiatrist for a proper diagnosis and to determine the treatment regimen that is right for you.
What Causes a Plantar Fibroma?
While there are no specific causes identified, a plantar fibroma can possibly come from genetic predisposition or the formation of scar tissue that forms from healing the tears in the plantar fascia.
What Are the Symptoms of a Plantar Fibroma?
There will be a noticeable lump in the arch of the foot that may or may not cause pain. If pain is felt, it is typically because a shoe is rubbing up against the lump or when walking or standing barefoot.
Treatment and Prevention
A plantar fibroma will not disappear without treatment, but it can get smaller and be a non-issue. If pain persists, a podiatrist examines the foot and when the arch of the foot is pressed, pain can be felt down to the toes. An MRI or biopsy might be performed to help diagnose or evaluate the plantar fibroma. The following non-surgical options are generally enough to reduce the size and pain of these nodules:
Surgery is considered if the mass increases in size and the patient continues to feel pain after non-surgical methods are tried.
If you have any questions please feel free to contact our office located in Wilmington, OH . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Bunions are large bony bumps at the base of the big toe. Medically known as hallux valgus, a bunion is a misalignment of the metatarsophalangeal joint, or big toe joint. The misalignment will generally worsen with time if left untreated.
The exact cause of bunions is unknown, with genetics seen as a potential cause. High heels and poorly-fitted footwear, rheumatoid arthritis, and heredity all seem to be potential factors behind the exacerbation of bunions. Women have been found to be more likely to develop bunions in comparison to men.
Bunions do not always produce symptoms. The best way to tell is if the big toe is pushing up against the next toe and there is a large protrusion at the base of the big toe. You may or may not feel pain. Redness, swelling, and restricted movement of the big toe may be present as well.
Podiatrists use a variety of methods to diagnose bunions. If there are symptoms present, podiatrists will first consider that it is a bunion. If not, a physical examination will be conducted to check function of the big toe. Finally, an X-ray may be taken to view the extent of the bunion and confirm it is a bunion.
Typically, nonsurgical methods are used to treat bunions, unless the bunion has become too misaligned. Orthotics, icing and resting the foot, roomier and better fitted shoes, taping the foot, and pain medication are usually utilized first. If the bunion doesn’t go away or causes extreme pain, surgery may be required. Surgeons will either remove part of the swollen tissue or bone to straighten the toe out.
If you have a bunion, it is recommended to see a podiatrist. The longer it is left untreated, the worse it may get. Podiatrists can properly diagnose and treat a bunion before it gets worse.

A bunion is a deformity of the joint at the base of the big toe. Bunions develop when the first metatarsal bone of the foot turns outward and the big toe points inward toward the other toes. This causes the joint to extend out from the foot. A bunion can become painful and interfere with walking and exercising as the joint becomes inflamed. It can be difficult to find shoes that accommodate a bunion, and it is best to avoid any additional pressure on the misaligned joint. Women are more likely to develop bunions because they tend to wear narrow shoes and high heels. Bunions can also be genetic and may result due to abnormal foot structures and shapes. Those with low arches and loose joints or tendons, as well as people who stand on their feet for prolonged periods, are also at increased risk for developing bunions. If you have a painful bunion, it is suggested you see a podiatrist who can provide alternative treatment options to help you live more comfortably.
If you are suffering from bunion pain, contact Dr. Gerald Perelman of Ohio. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
Symptoms
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our office located in Wilmington, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blisters are small pockets of fluid that occur on the top layers of the skin for several reasons. Friction, burns, and diseases are all known causes of blisters. Smaller blisters are known as vesicles, while larger blisters are referred to as bulla. The fluid inside the bubble can be blood, pus, or serum; which is a clear liquid that protects the skin. In most cases, blisters are not a major health issue, but they can be an indicator of a more serious condition.
Causes of blisters vary. Blisters are commonly caused by wearing poorly fitted shoes that rub against the foot. However, there are many other causes besides from friction; including burns, sunburn, insect bites, frostbite, poison ivy/oak, chemical exposure, impetigo, eczema, viral infections, and more.
Most blisters heal by themselves and do not require immediate medical care. If you have a blister, do not pop it since this may cause infection; it is advised to put a bandage over the blister to protect it. If the blister is large, causes pain, or if you have a fever, it is recommended that you see a doctor who can provide proper care. Blisters are easy to diagnose, and if considered prudent by the doctor, can easily be drained of fluid with a sterile needle as well.
To prevent blisters on the feet, wear shoes that fit properly and don’t cause rubbing. Socks can help prevent friction and it is recommended that you wear them if you are wearing shoes. Hand blisters can be avoided by wearing gloves during activities that cause friction against the hand. If you have a blister that pops, do not remove the dead skin, wash the area, apply antibiotic ointment, and cover with a bandage. It is okay in most cases to not seek immediate medical care for a blister if it was just caused by friction. However, if the blister causes pain or does not go away, it is suggested that you see a doctor for a diagnosis.

Blisters on the feet are pockets of fluid that form beneath the top layer of the skin to protect the lower layers from damage. Blisters on the toes, feet, or heels may be caused by friction, usually from pressure or rubbing against the inside of a shoe. Generally, a blister is filled with clear serum, but sometimes it may be filled with blood, or even pus if it becomes infected. As a rule, a blister will go away on its own in three to seven days. As new skin grows under the blister the serum will be reabsorbed into the body and the outer skin will dry up and flake off. However, it is important to remember that popping a blister can cause infection or inhibit the healing process. Wearing shoes that are comfortable and do not rub against the skin is a sure way of allowing a blister on the foot to heal, or preventing one from occurring in the first place. If you have a particularly painful blister, or one that appears to be infected, please make an appointment with a podiatrist. Antibiotics may be prescribed to ward off the infection, and the podiatrist may safely drain the blister in a sterile setting.
Blisters may appear as a single bubble or in a cluster. They can cause a lot of pain and may be filled with pus, blood, or watery serum. If your feet are hurting, contact Dr. Gerald Perelman of Ohio. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters are often the result of friction. This happens due to the constant rubbing from shoes, which can lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
Symptoms
(Blister symptoms may vary depending on what is causing them)
Prevention & Treatment
In order to prevent blisters, you should be sure to wear comfortable shoes with socks that cushion your feet and absorb sweat. Breaking a blister open may increase your chances of developing an infection. However, if your blister breaks, you should wash the area with soap and water immediately and then apply a bandage to the affected area. If your blisters cause severe pain it is important that you call your podiatrist right away.
If you have any questions, please feel free to contact our office located in Wilmington, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.